Beyond Kegels: Why Your Postnatal Workout Plan Might Be Missing the Pelvic Floor
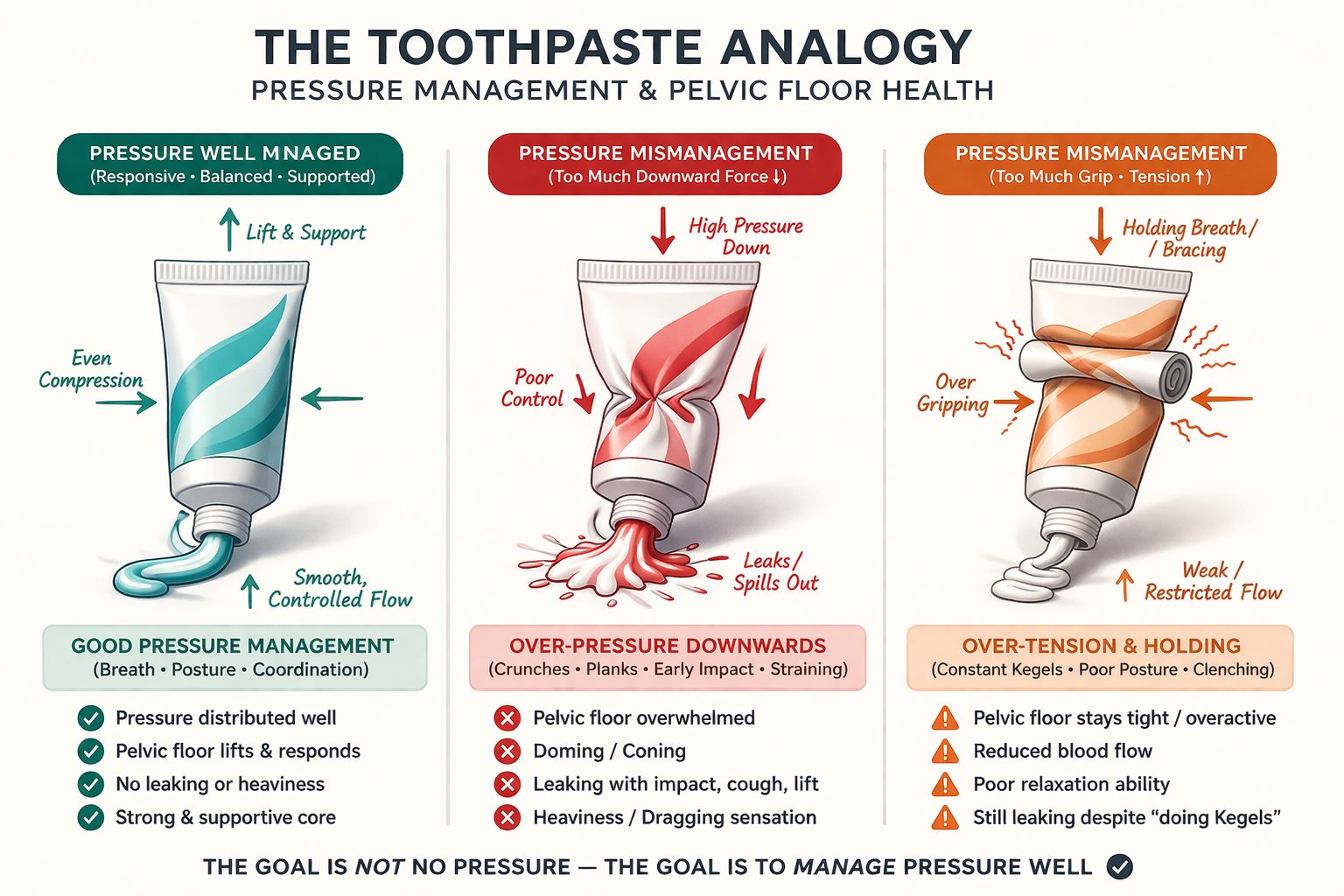
Visual showing how the Hypopressives Method helps manage pressure compared with bracing and chronic gripping in postnatal recovery.
If you are postnatal and still leaking, feeling heavy, or wondering why your middle does not feel as supportive as you expected, you are not alone.
Most women are told some version of the same thing after birth: do your Kegels.
And pelvic floor muscle training does matter. Evidence supports postpartum pelvic floor muscle training for reducing the odds of urinary incontinence and prolapse symptoms in the first year after birth.
But that is only part of the story.
Because many postnatal women are not simply weak. They are often carrying too much tension through the pelvic floor, abdominal wall, ribs, glutes, jaw, and breath. They are managing a body that has adapted to pregnancy, birth, feeding, lifting, poor sleep, stress, and postural change for months. In that context, isolated squeezing alone does not always restore true function. If the system is already overheld, more gripping can sometimes reinforce the very pattern that is preventing good coordination. NHS guidance for overactive pelvic floor is clear that if the muscles are both tight and weak, the tension should be addressed before the weakness.
This is where many women hit the Kegel ceiling.
They are doing what they were told. They are squeezing every day. But they still leak when they run, still feel heaviness, still notice doming through the abdominal wall, or still feel disconnected from their core.
That is why a good postnatal workout plan needs to go beyond voluntary tightening. It needs to restore timing, recoil, pressure management, and reflexive support. That is where the Hypopressives Method can become the missing link.
The real issue is not just strength. It is pressure management.
Pressure is not the enemy.
Pressure is always changing. It shifts with every inhale, every exhale, every lift, every cough, every hormonal fluctuation, every stress response, and every posture. The goal is not to create a body with no pressure. The goal is to create a body that can manage changing pressure well.
After pregnancy and birth, that pressure system is often less well organised. The pelvic floor, diaphragm, abdominal wall, and spinal support system may not be coordinating as efficiently as they once did. When that happens, a woman may start to feel symptoms when load or force exceeds what the system can distribute well.
Think of the tube of toothpaste analogy. If force is repeatedly directed downward into a system that is already under strain, something has to give. You may see doming or coning through the tummy. You may feel heaviness or dragging. You may notice leaking with impact, coughing, or lifting.
This is why traditional core exercises are not always the best starting point. Crunches, planks, aggressive bracing, and returning to impact too early can add load to a body that has not yet regained coordination. Postnatal return-to-exercise guidance commonly recommends a graded build-up, with caution around strain, breath-holding, and early impact, and suggests waiting until at least around 12 weeks before returning to running.
So the problem is not that women should avoid pressure forever.
It is that many women need help learning how to organise and shift pressure more effectively before they add more of it.
Beyond the squeeze: why reflexive strength matters
Your pelvic floor is not meant to work only when you think about it.
It is meant to respond automatically when you cough, laugh, pick up the baby, carry the car seat, push the pram uphill, or land from a jog. That is reflexive strength. And that is very different from lying still and doing repeated squeezes in isolation.
The Hypopressives Method offers a more systemic route into recovery.
Rather than asking the body to grip harder, it uses posture, breath mechanics, rib expansion, and where appropriate apnoea, to help the body manage and redistribute pressure more effectively. Great exhales, more functional inhales, and better postural organisation all contribute to a more responsive canister. Apnoea, when taught well and used appropriately, can be one part of that strategy.
For many women, this feels less like “doing more” and more like finally giving the body a chance to reorganise.
This is especially important in women who have become over-pressurised over time. The pelvic floor, lower back, and abdominal wall may not simply be weak. They may be carrying months or years of poorly directed force, gripping, bracing, and compensatory holding. In that situation, the work is not just about strengthening. It is about decompressing a system that has been under pressure for a long time so it can recover more efficient support.
Research on hypopressive exercise is still developing, but systematic review evidence suggests it can improve pelvic floor symptoms and may produce effects that are equal to pelvic floor muscle training in some measures and less than PFMT in others.
That matters, because it supports a more nuanced conversation.
This is not about saying Kegels and traditional PFMT are wrong.
It is about recognising that for some women, especially those already holding too much tension, isolated squeezes are not the full answer.
Healing the gap: diastasis recti repair from the inside out
This matters for women worried about abdominal separation too.
Diastasis recti repair is not simply about pulling the muscles together harder. It is about restoring tension, fascial responsiveness, and load transfer through the abdominal wall.
Evidence supports postpartum abdominal exercise training for reducing inter-rectus distance. But clinically, the issue is often bigger than the width of a gap. Many women need better tension through the linea alba, better breath mechanics, and better deep abdominal support.
This is where the Hypopressives Method can be helpful.
Lateral rib cage expansion, postural length, and diaphragm-led organisation can help the deeper abdominal system respond without relying on the same bracing strategies that often make women feel more pressure rather than more support. For many women, the tummy begins to flatten and firm from the inside out, not because they are sucking in, but because the whole system is beginning to work together more intelligently.
That is a very different kind of postnatal core recovery.
It is not just nor ever is about more gripping.
It is at its centre restorative function.
The missing link before impact
A lot of women do not just want to feel a bit better. They want a safe, confident return to the things they love.
Running. Lifting. Classes. Strength work. Jumping. Feeling capable again.
That is why the Hypopressives Method can be such a useful bridge in a safe return to exercise after baby.
It can help a woman rebuild auto-elongation while lifting baby gear, improve her ability to breathe under load, and test whether the system can manage everyday pressure before moving into higher-impact work. It can sit between early rehab and full performance.
That bridge matters.
Because a body that leaks with a cough, feels heavy after a walk, or domes when lifting the baby is not failing. It is communicating that the pressure system needs more support before impact is layered on top.
A better question than “Am I strong enough yet?” is often:
Can I cough without leaking?
Can I carry without bearing down?
Can I breathe well while I lift?
Can I move through the day without heaviness?
Those are meaningful signs of readiness too.
A 15-minute ritual for busy mums
The good news is that this does not have to be complicated.
A realistic daily practice might take 15 minutes:
a postural reset
rib expansion breathing
gentle pelvic floor awareness
a brief vacuum-based or apnoea sequence if appropriate
a short integration rest
No equipment. No long workout block. No all-or-nothing pressure.
For busy mums, consistency often matters more than intensity. Small daily inputs can change a lot when they are targeted and repeatable. That is why online core rehab for mums can work so well. It allows women to rebuild coordination in a way that fits real life, not just ideal conditions.
Why specialist guidance matters
Hypopressives are not just “suck your stomach in and hold your breath.”
Done badly, women can grip the throat, flare the ribs, bear down into the pelvic floor, or substitute one pressure problem for another. That is why specialist guidance matters.
A woman recovering from a C-section may need different pacing and scar-sensitive support than someone recovering from a vaginal birth. A woman with diastasis, prolapse symptoms, rib gripping, or pelvic floor overactivity will need a different entry point again.
That is why working with a postnatal exercise specialist Scotland or finding Hypopressives classes Edinburgh or online can make such a difference. It is not just about exercises. It is about assessment, pressure strategy, posture, timing, and knowing what the body in front of you actually needs.
The wider postnatal physiotherapy approach supports this too: graded return, symptom awareness, pelvic floor assessment, and not rushing into strain or impact before the system is ready.
Beyond Kegels
Your postnatal recovery is not about working harder.
It is about working more intelligently.
Kegels can absolutely help. But for many women, the missing piece is not more squeezing. It is learning how to come out of chronic gripping, manage changing pressure better, and rebuild support as a reflex rather than a constant conscious effort.
That is what the Hypopressives Method can bring to a well-designed postnatal workout plan.
Not fear.
Not force.
Not endless squeezing.
Just a better managed pressure system, a more connected core, and a smarter route back to strength.
Ready to move beyond Kegels? Join my Postnatal Power Workshop, Pelvic Floor MOT or begin 1:1 coaching with Hypopressives Scotland to rebuild your core safely, confidently, and in a way that actually fits a postnatal body.
FAQs
How soon after birth can I start Hypopressives?
Usually after your 6-week GP or postnatal check for exercise progressions, though gentle breathing and awareness work may begin earlier with appropriate guidance. Group exercise and gym return are commonly advised after that early check, with a gradual build from there.
Can I do these after a C-section?
Yes, with appropriate modification and progression. Scar healing, comfort, and individual recovery all matter. General NHS guidance supports gradual progression of pelvic floor and basic core work in the early postnatal period, with bodyweight and low-level strengthening introduced progressively.
What if I already do Pilates?
Pilates can be excellent. Many women simply find that Hypopressives add a more specific focus on pressure management, breath organisation, and reflexive lift.
Do I have to do the vacuum to see results?
No. Apnoea can be a powerful tool, but better exhales, better inhales, posture, and rib-pelvis organisation can all improve coordination and support.
CTA box
Beyond squeezing. Back to support.
If your body still feels heavy, leaky, or disconnected after birth, it may not need more gripping. It may need better pressure management, reflexive core support, and a smarter way back to movement.
Explore my Pelvic Floor MOT or book 1:1 coaching with Hypopressives Scotland.