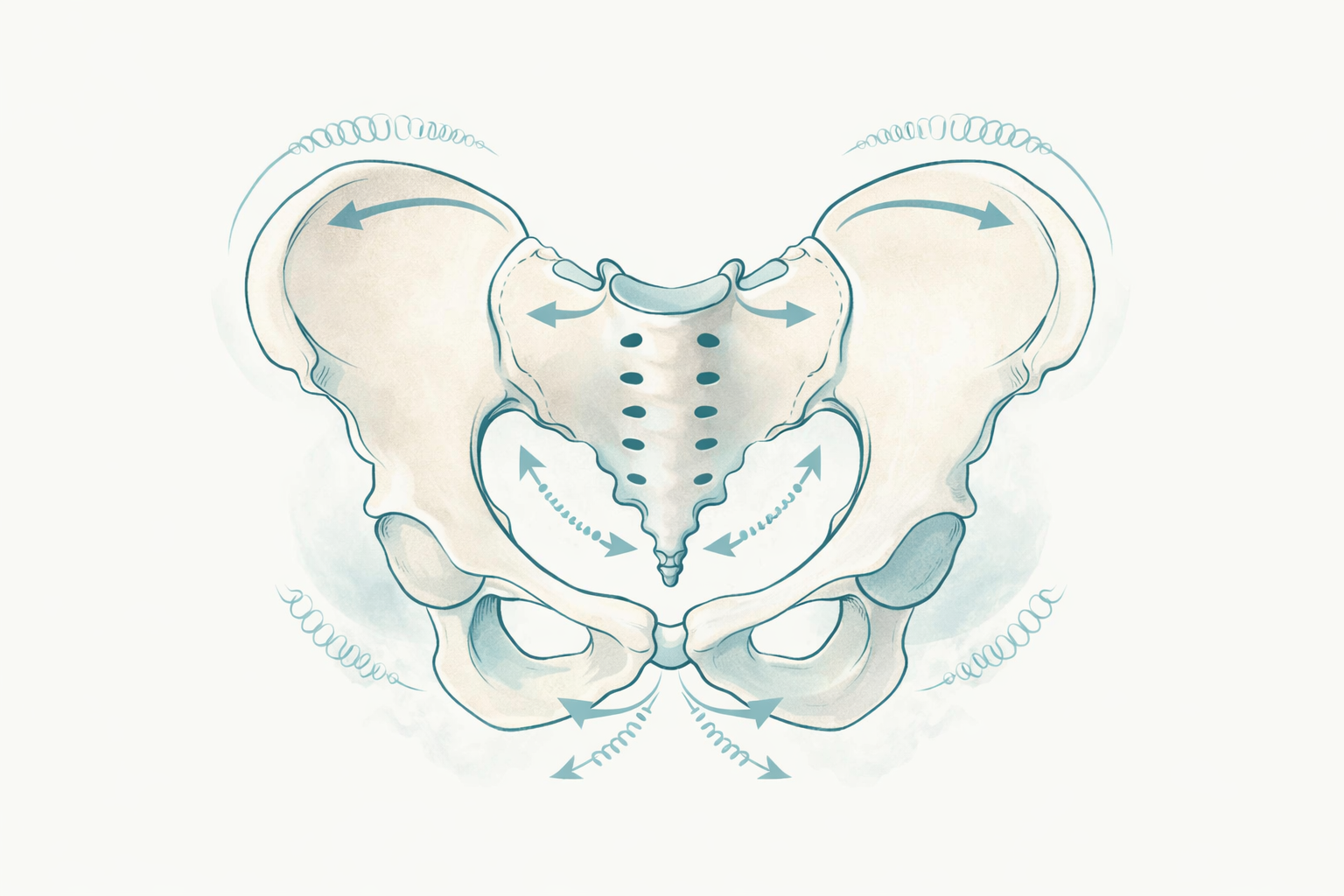
Why the ilia and sacrum need to move
The pelvis is designed for subtle, responsive movement. Small movement between the ilia and sacrum helps the body absorb and transfer force more effectively.
Elasticity, viscoelasticity, and the pelvic floor
When people think about pelvic floor health, they often think about the muscles alone.
But the pelvis is not just a bowl of muscles. It is a living ring of bones, fascia, ligaments, joints, and pressure relationships. If we want the pelvic floor to feel more supported and less overloaded, we need to care about how the two ilia and the sacrum are moving together. The sacroiliac joints sit between the sacrum and ilia and are designed to transfer load between the spine and legs. They are built for stability, but not for total stillness. Many of my clients have been, like I was before all of this, blissfully unaware that there is any movement in the pelvis itself.
It is not dramatic movement.
There are no big visible wobbles.
But there are subtle, responsive, well-timed movements.
Because that is how the pelvis is designed to work.
The pelvis is not meant to be rigid
One of the most useful ideas here is viscoelasticity.
Living soft tissues are not purely stiff and they are not purely fluid. They show both elastic behaviour, meaning they can store and release some energy, and viscous behaviour, meaning they also change over time when load is sustained. overviews of fascia and connective tissue describe classic viscoelastic features such as creep (visualise thick toffee slowly lengthening) and stress relaxation, and broader mechanobiology research shows that living tissues respond and adapt to the mechanical environment around them.
This is why thinking about the ligaments as being like “rubber bands and thick oil” as an image is so helpful.
A rubber band gives you spring and recoil.
Thick oil gives you slow flow.
Human connective tissue has elements of both. That does not make the body weak. It makes it adaptable. But it also means that if tissue is held under poor load for long enough, it can gradually change. In viscoelastic tissues, prolonged strain can produce creep, meaning gradual deformation over time, while stress relaxation describes a fall in internal stress when tissue is held at a fixed length.
So if the pelvis is repeatedly held in a collapsed, tucked, braced, or one-sided pattern, the tissues around the sacrum and ilia are not passive bystanders. They are going to be responding to that history of load.
Why small movement matters
The sacroiliac joints do not need very much motion to matter. A systematic review found that normal sacroiliac joint motion is small, commonly measured in low degrees rather than large visible ranges, but that small motion is still biomechanically meaningful. The joint helps transfer bending moments and compressive loads from the trunk into the pelvis and lower limbs.
That is important because walking, changing weight from one leg to the other, rising from a chair, bending, carrying, and breathing all ask the pelvic ring to respond. The pelvis is not meant to behave like a frozen block. It needs enough support to transfer force well and enough movement to adapt to that force, the goldilocks formula. This is one of the central ideas in sacroiliac joint function: a balance of stability and mobility, sometimes described as form closure and force closure.
In simpler language, the pelvis needs structure and responsiveness at the same time.
What this means for the pelvic floor
The pelvic floor does not work in isolation. It is part of a broader pressure and force system involving the diaphragm, abdominal wall, spine, pelvis, hips and feet. If the pelvic ring cannot subtly adapt, other tissues often try to compensate. That can show up as gripping through the glutes, stiffness in the lower back, poor pressure sharing through the trunk, or a pelvic floor that feels as though it is always “on” or always trying to do too much. The sacroiliac joint literature and studies repeatedly describe the pelvis as a key load-transfer region between the lumbar spine and lower extremities, which helps explain why whole-body organisation really matters here.
That does not mean every pelvic floor symptom comes from sacroiliac movement. Bodies are more complex than that. But it does mean the pelvic floor tends to do better when it is part of a coordinated system rather than left to manage pressure and force alone.
Fascia, ligaments, and glide
Fascia is not just wrapping. It is a connective network with mechanical and sensory functions, and research discussions from fascia congresses I have been on and reviews I have read describe its viscoelastic behaviour and its ability to adapt to tension, shear, and compression. When fascia and ligaments are loaded in one direction for too long, they can show creep and altered tension patterns.
This is where the image of a rubber band that becomes more elongated under heat and prolonged pull ,that I borrowed from one of Eric Franklin’s books, can truly help us to understand that living tissue is not fixed. It can lose some of its ideal rebound if it is constantly pulled in one direction without enough variation, support or recovery. Human tissue is more adaptable than rubber because it is alive, but the principle still helps: time under strain matters.
This is also why scar tissue and adhesions can matter. The "Pull" Concept: This is a core theme of Bowman's work is how mechanical "loads" and restrictions, like those created by scar tissue, pull on our cells and change how our body moves. She explains that scar tissue isn't just a surface mark but a three-dimensional "snag" that creates a pull through the entire fascial web and it is fair to say that restrictions in connective tissue can alter local glide and change how force travels through the wider system. Since fascia and other soft tissues are mechanically responsive, their organisation influences how movement and load are distributed.
Why walking is such good medicine
Walking is one of the simplest and most natural ways the body rehearses pelvic organisation.
Each step asks the pelvis to receive load, transfer force, coordinate with trunk rotation, and respond to ground reaction forces. The sacroiliac joint is part of that chain. It does not need huge movement to contribute. It needs meaningful movement. Reviews of sacroiliac joint anatomy and function consistently describe its role in effective load transfer between spine and legs, which is exactly what walking depends on.
Done well, walking can help the pelvis remember rhythm.
It can help the ilia alternate.
It can help the sacrum respond.
It can help the system reclaim a little spring and rebound.
That is one reason I so often come back to gait, posture and breath before simply adding more “pelvic floor exercises”.
This is not about making the pelvis loose
This part matters.
The answer definitely is not a floppy pelvis., gosh no.
It is also not endless stretching.
Neither is it hanging into ligaments.
And it is not trying to force movement into the sacroiliac joints.
The answer is a pelvis that can adapt.
That means enough movement to absorb and transfer force, and enough support to stay organised under load. The joint functions best when stability and mobility coexist.
What I look for in practice
When I watch someone breathe, walk, stand, squat, or shift weight, I am often asking:
Does the pelvis behave like a living ring, or a rigid block?
Can one side accept weight without the whole body bracing?
Is there spring through the system, or just tension?
Can the sacrum and ilia respond subtly, or does everything feel held?
Does the pelvic floor look supported by the whole body, or left to do too much on its own?
Those questions matter to me far more than whether someone can produce a strong squeeze in isolation.
The hopeful part for all of us humans
Living tissues adapt. Which is just the best news.
That is the whole point around what I do and what my clients practice.
Mechanobiology research shows that tissues are shaped by load and that growth, remodelling and repair are influenced by the mechanical environment. That means poor loading patterns can create problems over time, but better and improved loading patterns can also help the system recover capacity.
So if your pelvis has become a bit rigid, tucked, braced, or one-sided, that is not the end of your story it’s the middle. We still have space for an epilogue and then a finale!
Through better breath, better posture, walking, gentle pelvic movement, whole-body strength work, fascial hydration and glide, and calmer nervous system input, the body can often find a better relationship with gravity again. That is when the pelvic floor often starts to feel less overworked and more supported.
Final thoughts
The ilia and sacrum do not need dramatic movement. But they absolutely need meaningful movement.
Small movement.
Shared movement.
Timed movement.
Movement that lets the pelvis absorb, transfer and return force.
Because the pelvis is not meant to be a dead weight hanging from the bottom of the spine. It is a dynamic, living centre.
And the more we understand elasticity and viscoelasticity, the more clearly we can see this:
Pelvic floor health is not just about strength.
It is about spring.
It is about glide.
It is about timing.
It is about how well the whole body meets gravity.
If your body feels heavy, tense, disconnected or as though your pelvic floor is trying to do too much, my Pelvic Floor MOT looks at the bigger picture of you, the middle of your story- breath, posture, movement, pressure and tension patterns - so we can make sense of what your body may actually need. Then we work on what that looks like for your epilogue and then you will have the tools to write your finale all by yourself - how bloody powerful is that!
And if you are ready to begin more gently, my £29.95 beginner course is a simple place to start exploring release work, breath and the foundations of Hypopressives.
Try this: a gentle pelvic dance to wake the pelvis up
If all of this feels a little theoretical, here is a simple way to begin feeling these ideas in your own body.
This short sequence is not about forcing movement or “mobilising” the pelvis aggressively. It is about helping the feet, legs, ilia and sacrum begin to talk to each other again. It invites rhythm, softness, weight shift and subtle pelvic motion, all the things a responsive pelvis tends to like.
Pelvic Dance: Feet to Pelvis Flow
5–7 minutes
Stand with your feet about hip-width apart.
Keep the knees soft.
Let your arms hang easily by your sides.
Take a moment to feel the ground beneath you.
There is no effort here.
You are not correcting yourself.
You are simply waking the body up.
1. Gentle prancing through the feet
Begin by gently prancing through the feet, one foot at a time.
Let one heel lift as the other settles.
Then switch.
It is almost like a soft jog on the spot, but without leaving the floor.
Feel the weight shift.
Feel the ankles, calves and soles of the feet responding.
This is about rhythm, not height.
Light. Easy. Springy.
Stay here for 30–60 seconds and let the movement travel naturally up into the legs and pelvis.
2. Pelvic tilts
Now bring your awareness to the pelvis.
Gently tilt the pelvis forward…
and back.
Like a small bowl of water tipping and pouring.
Nothing forced.
Just a smooth rocking motion.
Repeat 4–6 times, slowly and fluidly.
3. Side-to-side pelvis
Now let the pelvis move side to side, as if it is gliding along the horizon.
Right…
Left…
Imagine your pelvis floating on calm water.
Repeat 4–6 times.
Let the upper body stay relaxed.
4. Hip hikes
Now lift one side of the pelvis slightly.
Then let it release down.
Switch sides.
It is subtle.
Almost like shrugging one hip at a time.
Right hip up and down.
Left hip up and down.
Repeat 4–6 times each side.
No gripping in the glutes.
Let it feel playful and light.
5. Rotational flow with step
Step the right leg slightly forward.
Let the toes turn gently towards the left as your arms and torso rotate to the left.
Then bring the leg back,
let the toes turn to the right,
and rotate the arms and torso to the right.
So the pelvis, legs and arms are all spiralling together.
Like slowly wringing out a towel.
Repeat 4–6 times.
Then switch sides and repeat with the left leg forward.
6. Coccyx figure of eight
Now imagine your coccyx is a long pencil pointing down towards the floor.
With that pencil, begin to draw a figure of eight on the ground.
Let the pelvis lead.
Keep the legs soft and responsive.
Make the movement smooth and continuous.
Draw the figure of eight 4–6 times in one direction.
Pause.
Then repeat 4–6 times the other way.
Let this feel sensual, fluid and curious rather than like exercise.
Pause
Finish by standing still for a moment.
Notice:
your feet
your pelvis
your breath
This is your body saying:
I’m awake.
I’m safe.
I’m ready to move.
Add this too: spine awareness standing bend
You can follow the pelvic dance with this simple standing bend to notice how the sacrum and spine respond together.
Stand with your feet about hip-width apart.
Soften your knees, not into a squat, but as if you are gently lowering yourself.
As you begin to lower, notice what your spine is doing.
Feel how the lower curve deepens slightly as you go down.
Notice how the sacrum tips gently forward and draws back.
Then slowly come back up to standing.
As you rise, feel the sacrum tip back at the top,
the apex of the curve draw in,
and the spinal curve become shallower again.
Almost like pressing down on a spring and then releasing it.
At first, let the breath be natural.
Then, if it feels easy, add:
Inhale as you lower
Exhale as you come back up
Let it stay slow, fluid and easy.
This is not about effort.
It is about awareness.
Sometimes the pelvis does not need more gripping, squeezing and harsh treatment. What It needs is a better conversation.
More rhythm.
More response.
More space to share load well.
This kind of gentle movement can be a simple place to begin. You are very, very welcome.